subperiosteal implant
If jawbone atrophy is significant and prevents patients from receiving traditional implants, a subperiosteal implant is recommended. This method, as old as dentistry, has resurfaced with technological progress and can provide customers previously dependent on dentures or bone procedures with hope to eliminating their limitations.
What Is a Subperiosteal Implant?
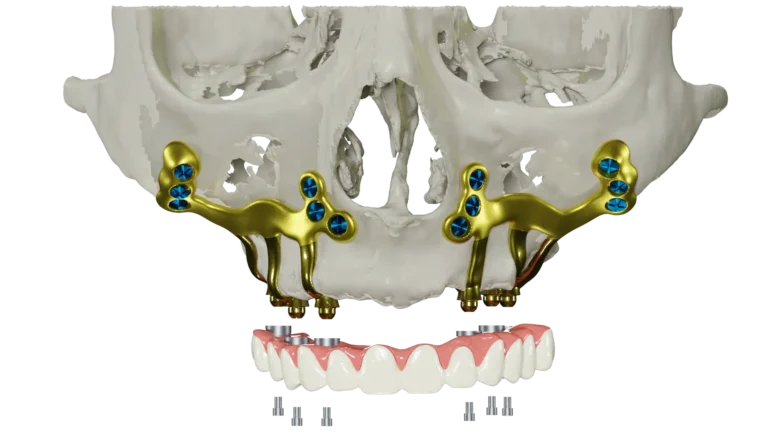
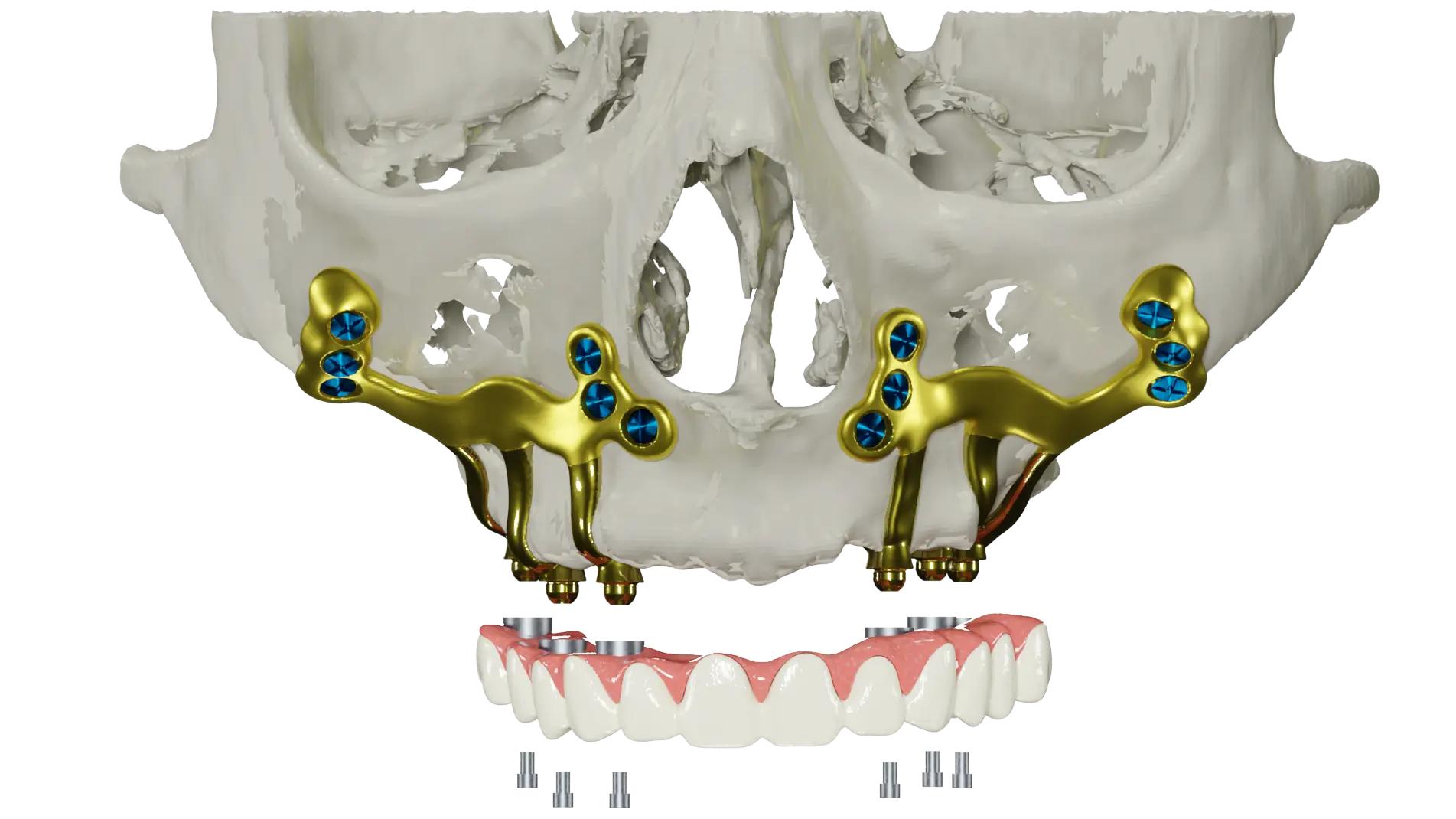
In subperiosteal implants, a custom-made titanium framework is placed atop the jawbone beneath the periosteum (the gum tissue). Unlike traditional dental implants, small posts stick through your gums to” anchor” replacement teeth, bridges or full-arch prosthetics. This custom-fit framework is made possible by advanced imaging [cone-beam computed tomography (CBCT)] and design/manufacturing technology (CAD/CAM) that determine the precise contours of the jaw at the individual patient level.
This design does not require drilling deep into the bone, which is advantageous when the patient lacks sufficient bone height or density. Over time, the implant integrates with surrounding tissues because it does not require bone volume for anchorage and provides stable support for prosthetic teeth.
A Very Brief History of Subperiosteal Implants
The roots of subperiosteal implants can be traced back to the 1940s, when Swedish dentist Dr Gustav Dahl pioneered this technique. In the United States, it became widely popular through Goldberg and Gershkoff’s findings and, until the end of the 1980s, was one of the first approaches for edentulous patients with atrophic jaws. The early versions were made with cast metal frameworks and had decent success for their time.
The late 1960s then heralded a seismic shift in this direction with the introduction of osseointegrated endosteal implants pioneered by Dr Per-Ingvar Brånemark. Higher long-term complication rates with subperiosteal options and improved predictability of root-form implants contributed to the decline. Today, new interest comes from digital workflows, 3D printing, and use in oncology reconstruction or in extreme atrophy cases where other solutions do not work.
Who Is a Good Candidate for a Subperiosteal Implant?
For patients with extensive mandibular or maxillary bone loss due to periodontal disease, long-term denture use, trauma, or tumour resection, subperiosteal implants are appropriate. They help those who cannot or prefer not to undergo bone grafting surgery and have certain medical conditions that prevent invasive surgery, as well as those who do not have enough bone for endosteal implants.
Candidates mainly include older adults with significant resorption, patients requiring the rehabilitative full-arc of teeth, and those with congenital jaw deficiencies. Suitability is determined through a detailed examination with an oral surgeon or implant specialist, review of medical history and CBCT scans. Healthy gums and overall oral hygiene are essential, as with any implant, long-term success will require both.
Step-by-step guide to the Subperiosteal implant procedure
It all starts with in-depth diagnostics. i.e., impressions/CBCT scans/digital modelling create a custom titanium framework tailored to the individual patient.
The dentist makes an incision in the gum tissue during surgery, typically performed under local anaesthesia or sedation, to expose the jawbone. Small screws are used to fix this custom framework in place. The gums are then stitched over the protruding posts. In certain contemporary protocols, provisional prostheses may be fixed straight away or within hours of placement.
Healing is generally a matter of weeks to months, as soft tissue undergoes remodelling and the framework stabilises. Once integration takes place, a secondary minor procedure can connect the final prosthesis. The whole schedule is usually shorter than bone-graft-plus-implant sequences, and many patients get functional teeth within weeks.
Key Advantages of Subperiosteal Implants
A key advantage is avoiding the need for bone grafting, which shortens surgery time and reduces cost and post-operative discomfort. The procedure is more minimally invasive with respect to bone manipulation, making it attractive to patients with health issues or limited time.
Custom-made ensures an exact fit to improve comfort and function for chewing, talking, and smiling. In some cases, subperiosteal implants restore facial structure and inhibit further resorption. These implant types are viable for single teeth, partial bridges, or full arches. Some newer designs increase durability, with some studies indicating beneficial results in particular patients. Recovery can be much faster than with multi-stage bone augmentation, and the solution provides a natural feel without the gum slippage commonly found in traditional dentures.
Potential Disadvantages and Risks
Subperiosteal implants: Pros and cons, despite advantages. Historically, they were associated with higher failure rates than endosteal implants due to difficulties with long-term tissue integration and cleaning around the framework. The most common implant failure is mucositis, or inflammation around the implant due to poor oral hygiene.
Although this technique avoids drilling into the bone, it requires skilled exposure of the jaw and accurate positioning of the framework, making it technically demanding. Patients may initially notice slight visibility of the posts of metal or a change in sensation. With appropriate care, patients can have a 10-15-year survival (or more!), But follow-up visits may be needed. The downside is that not every dental practice can provide this option.
Subperiosteal Implants Versus Endosteal Implants
Endosteal implants, titanium screws inserted directly into the jawbone, are still considered the gold standard because of superior osseointegration and longevity. They require sufficient volume and are often used in cases of bone deficiency before bone grafting.
Subperiosteal implants are amazing to use for those who lack bone, eliminating the need for grafting and shortening the passive treatment period. Endosteal options tend to be stronger and less prone to complications over time, while subperiosteal frameworks can provide good support when the anatomy is compromised. Dr Leach said the choice of whether to use one, two, or neither bone graft is based on how each one looks, his experience with them, and patient preferences. Many practitioners are now employing hybrid techniques or relegating subperiosteal implants to specific high-need scenarios.
Recovery, Aftercare, and Maintenance
Patients are often swollen, bruised, and sore after the procedure, but these effects can be treated with prescription medications. During the first stages of healing, a soft diet, antibiotics, and antimicrobial rinses to prevent infection are essential.
Once prosthetics are attached, general function returns gradually. Long-term success depends on good oral hygiene: brushing and flossing around the posts every day, as well as professional cleanings every three to six months. Tobacco avoidance and systemic health contribute to implant stability. Routine X-rays track integration and spot problems early.
Success Rates and Future Outlook
They show significantly greater implant survival compared to older generation subperiosteal implants that did not benefit from digital precision manufacture. Endosteal implants demonstrate more than 95% success at 10 years under ideal conditions, but appear to be less effective for retention, as shown by contemporary subperiosteal designs with tailored CAD/CAM endosseous components and roughened surface formations.
In fact, the market for these implants is accelerating worldwide and expected to grow steadily into the 2030s with advances in technology. Active studies are underway to establish bioactive coatings and hybrid design approaches to enhance integration and reduce inflammation. Subperiosteal implants are an important life-changing alternative that restores confidence and quality of life for people with advanced bone loss.
So, in summary, the subperiosteal implant is a custom-made, high-quality solution when the traditional method doesn’t work. Then make sure to consult a qualified implant dentist and to ensure that you have the correct expedient. If properly cared for, this method can provide long-lasting functional dentition and restored oral health that lasts for years.
You may also read nowitstrend.